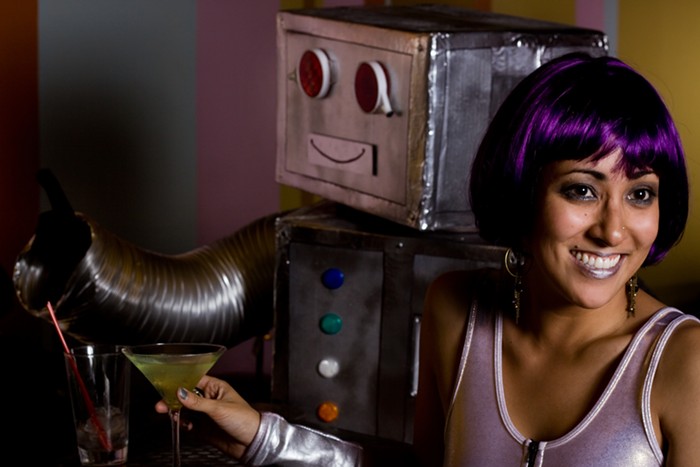When Brett Kavanaugh was confirmed to the Supreme Court in October, abortion advocates across the country sounded an alarm: There were at least 13 abortion-related cases that the now majority-conservative court could immediately rule on. Many of those cases threaten to overturn Roe v. Wade, the landmark legislation that protects women’s rights to safe and legal abortions.
Planned Parenthood responded to Kavanaugh’s confirmation by pinpointing 10 states with laws that make abortion relatively accessible, then prioritizing the organization’s work to strengthen and expand those laws. Its hope is that even if Roe is overturned, this network of pro-choice outposts would ensure that those living in states that ban abortion can still safely access the procedure.
Oregon, often singled out by reproductive rights leaders as the most pro-choice state in the country, was identified as one of those 10 states.
Abortion access in the US is already wildly inconsistent across state lines, making Oregon a destination for women seeking affordable and non- judgmental reproductive health care. But building a network like the one proposed by Planned Parenthood will require a surge in state funding, cooperation between multiple Oregon nonprofits, and improvements to Oregon’s reproductive rights policies—which, despite their relative strength, still have weak spots.
Jimmy Radosta, a spokesperson for Planned Parenthood Advocates of Oregon, said the organization’s plan to strengthen abortion access in Oregon is still “in the earliest stages.”
“About 20 states, including Idaho, would lose access to abortion if Roe v. Wade goes away,” says Radosta. “The goal, ultimately, is to make sure that no patients lose access to the care they need.”
Oregon has already laid the groundwork to meet that goal. In just the past year, Governor Kate Brown passed legislation requiring insurers to provide birth control and abortion procedures without charging a copay, while Oregon voters rejected a ballot measure that would have cut state funding for abortion costs.
It’s these progressive policies that encourage women to travel from less abortion-friendly states to Oregon. According to a recent report from the Centers for Disease Control and Prevention (CDC), 11 percent of all Oregon abortions in 2015 were performed on out-of-state patients, a number that’s consistent with recent years.
“The goal, ultimately, is to make sure that no patients lose access to the care they need."
“We’ve always seen patients from out-of-state here in Oregon,” says Paula Bednarek, the medical director of the Portland-based Planned Parenthood Columbia Willamette. “Oregon is a place of access for reproductive health.”
The CDC’s report didn’t track which states those patients came from, but according to Bednarek, many of Planned Parenthood’s out-of-state patients come from Idaho and Alaska.
Idaho bans third-trimester abortions and requires women to wait 24 hours between receiving state-mandated abortion counseling and receiving the procedure. Alaska also mandates counseling before the procedure and requires parental consent for patients under 18.
The CDC also didn’t track the distance that many in-state patients have to travel to get an abortion in Oregon. Bednarek said one of her patients—a teenager from Ashland—traveled 300 miles to Portland after being told there was a month-long wait for an appointment at her local clinic.
Even for those living in the Portland area, Oregon’s safety net for women seeking abortion isn’t without holes. Portland resident Beth Vial was 22 when she found out she was pregnant in 2017. For Vial, who has two chronic illnesses, the telltale signs of pregnancy were ordinary symptoms—meaning she didn’t know she was pregnant until her third trimester, 26 weeks into her pregnancy.
Third-trimester abortion is legal in Oregon, but neither Planned Parenthood nor the Lovejoy Abortion Clinic in Portland offer the procedure for women as far along in their pregnancy as Vial, because risk of the procedure causing physical harm to the patient rises dramatically after 24 weeks. A doctor at Oregon Health & Science University recommended Vial instead go to a clinic in in Albuquerque, New Mexico, that provides abortions for patients who are up to 28 weeks pregnant.
The abortion alone—not counting airfare, lodging, food, and the cost of taking two weeks off work—would cost Vial $10,500. Her insurance company offered to reimburse her $200.
“That gave me two weeks to compile the resources to travel down there, have a place to stay, feed myself, and then pay the deposit for the procedure,” she said.
Vial ended up getting help from friends, as well as from the Northwest Abortion Access Fund (NWAAF) and other organizations to pay for her procedure. As a white middle-class woman, Vial says she felt more privileged than many in her position; she is now a NWAAF board member and volunteer.
“Even though Roe exists, many people don’t have access to abortion.”
The volunteer-run NWAAF works to ensure that women in Alaska, Oregon, Washington, and Idaho who need an abortion aren’t prevented from receiving one because of cost or other barriers to access. In 2018 alone, the organization helped cover the cost of nearly 700 abortions and assisted with travel expenses for 125 patients.
“A lot of the time our callers are folks who choose between paying for basic needs like rent and groceries, or paying for their abortion care,” said Samantha Gladu, an NWAAF board member. “Even though Roe exists, many people don’t have access to abortion.”
NWAAF and its parent organization, the National Network of Abortion Funds, experienced what Gladu called a “Trump bump” in fundraising after the 2016 presidential election, but donations have slowed since.
When Planned Parenthood announced its plans for a 10-state network in October, Yamani Hernandez, the president of the National Network of Abortion Funds, tweeted her concern that Planned Parenthood was overlooking the efforts of local abortion funding organizations and ran the risk of duplicating efforts. Gladu says that locally, Planned Parenthood and the NWAAF do work together, but that as abortion access continues to be under threat, there’s more room for teamwork.
“Collaboration can look like shoring up the networks that already exist,” Gladu says. “Directing resources to the organizations who are already doing the work. In particular, the work removing financial and logistical barriers to abortion is really critical.”
Some pro-choice advocates are holding out hope. On December 10, the Supreme Court declined to hear a case regarding Medicaid funding for Planned Parenthood, allowing a lower court decision—one in favor of the organization—to stand. Kavanaugh was among the justices who refused to hear the case, prompting some to speculate he might not be as opposed to reproductive rights as many pro-choice advocates had feared.
But there are still a dozen abortion-related cases that the Supreme Court could choose to take up in the foreseeable future. With so much at stake, Oregon will continue to play a vital role in the fight for accessible reproductive care.
“We have to prepare for the worst,” Radosta says. “No matter what.”