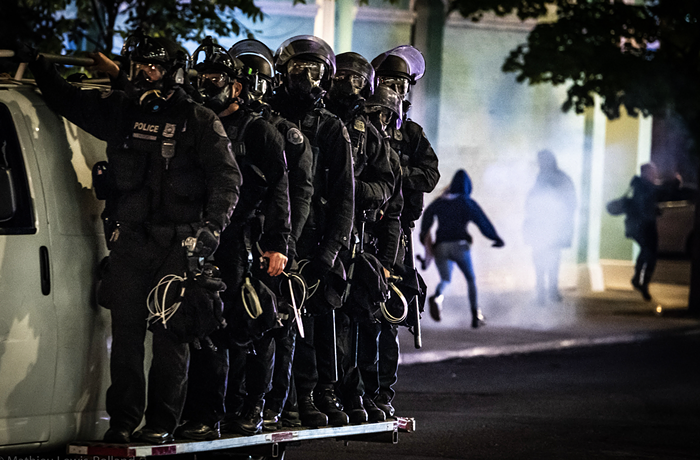On Friday night, Oregon Gov. Kate Brown was joined by Portland's top elected officials to announce next steps in the statewide response to COVID-19's spread. While Brown urged Oregonians to stay home, she didn't announce what many medical professionals had been hoping for: A clear order for members of the public to stay in their homes (referred to as "shelter in place" in other states that have already taken this measure) except for essential errands, work responsibilities, and solo exercise.
The press conference left Portlanders feeling like their elected leaders were not in alignment in an organized response to a global pandemic.
An hour before Brown's announcement, we spoke with an oncology nurse at a Portland hospital who raised concerns about what they perceive to be a dangerously unorganized response to COVID-19's spread—not just in their hospital, but across the state and country. The nurse asked to keep their identity and workplace private, fearing retribution from management for speaking out. Their perspective shines a spotlight on where a lack of transparency by leadership may be having the gravest impact. Here's the conversation:
MERCURY: What does a normal week look like for you?
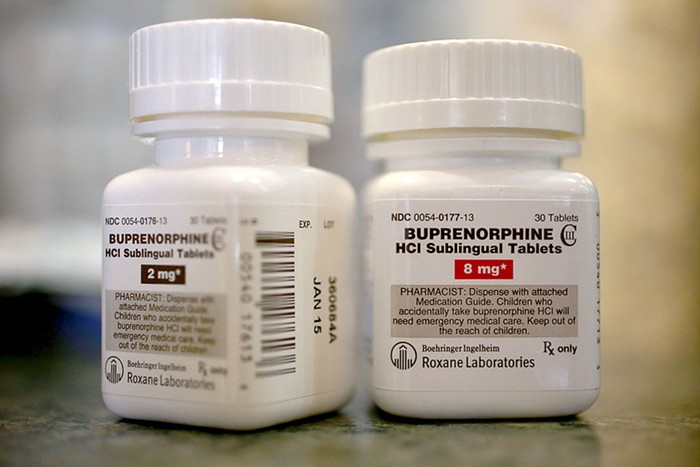
NURSE: I'm in the oncology department, where we see more than 100 patients every day for treatment. Some come in as frequently as every other day for chemotherapy treatment—it really depends on how severe their illness is. These are patients with incredibly weak or non-existent immune systems, meaning they're particularly vulnerable to the coronavirus.
What has your work been like this week?
Every patient we have to screen for COVID-19 as they come in. But the instructions we’re getting is changing hourly. As of this Monday, the oncology department finally had access to start testing our patients, who are severely immunocompromised, for the coronavirus. But for the past month and half, if one of our patients came in with severe respiratory issues and flu symptoms—and even if they had had contact with someone who had COVID-19—we still were being told to send them home.
Do you know if they’ve recovered?
A lot of patients we sent home I haven’t seen since. Some of them had to delay cancer treatment because they were sick. But when you have lymphoma, skipping a week could mean you’re going to be super unstable by the next week. It’s definitely affecting care. What’s scary is that I don’t know if they ended up in the hospital or if they ended up dying. Or maybe they recovered. We had no idea. We do know that we sent them back into the public with severe symptoms.
But you said that changed Monday, right? Now you can test your patients for COVID-19?
Yes, if they have major symptoms. I think it’s just the emergency department and oncology that can test right now. Family medicine is a different story. I have friends who are responsible for triaging calls for people through the family medicine clinics, and a lot of those people have a fever, dry cough, and trouble breathing—the symptoms of this virus. All they can do is tell them to stay home. The scary thing is that most of the people they’ve spoken with had been out in public that same day.
To be honest, me and my coworkers—other nurses—we’re stumped by this situation. We’re supposed to be on the front lines, but even we have had a hard time following who can and cannot get tested.
How is your hospital’s supply of protective medical gear holding up?
We’re running out of isolation gear and basic protective equipment. Thousands of boxes of masks have been stolen over the course of the month. It’s so strange: At least one person who was stealing them at night was taking the masks out of the boxes and recycling them before leaving. We’d come in the next day to a recycling bin filled with empty mask boxes.
By the end of next week, we’re anticipating that every major hospital in Portland will be out of protective equipment. We’re expecting donations, I’ve heard, but we don’t think it’s going to be enough.
Do you think the public and government officials are taking this seriously enough?
I personally feel protective over my oncology patients, since they’re so vulnerable. We have some patients who have both HIV and lymphoma, making them ever more immunocompromised. They’re frightened, and I’m frightened for them.
Here’s what I know: COVID-19 is really, really contagious and it’s not presenting the same across different demographics. It’s clear the most vulnerable are going to get the sickest and, eventually, probably everyone will get sick. Our immune system just doesn’t sense it early enough. It’s not airborne, meaning that unless you’re right in front of someone’s face [and they sneeze or cough on you], you’re fine. But the virus stays on surfaces for a very long time.
[Editor's note: The nurse later clarifies that COVID-19 is spread through droplet transmission, which means it can still be suspended in the air after someone coughs—just not nearly as long as a virus that is airborne.]
The people who are walking around with their dog I’m not concerned with. What worries me is that, we have great critical care here [in Oregon], but we have awful primary care. Across the country, our health care system isn’t set up to give people access to the kind of preventative care they need. Which means our whole country is at risk for complications. And we’re not prepared to care for them all.
Anything else you want to add?
I hope everything I’m telling you isn’t true. This is just my understanding, from my specific perspective at my job. I am eager to be proven incorrect. But [local and national government] has been acting perplexed about what this is for months. I think people deserve to know that it’s really out there. It's something we need to be concerned about.